The Alarming Rise of Vibrio vulnificus Amidst Climate Change: A Near-Fatal Case Underscores Urgent Public Health Threat
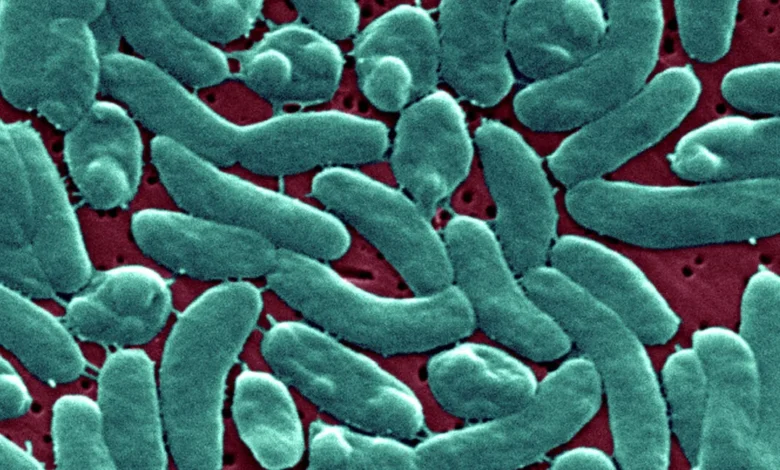
The harrowing survival story of a man who lost his leg to a virulent Vibrio vulnificus infection has brought into sharp focus the escalating danger posed by this "flesh-eating" bacterium, a threat magnified by the accelerating impacts of climate change. His experience, detailed in a recent medical case study, serves as a stark warning of the pathogen’s devastating potential and its expanding geographic footprint, prompting medical experts to label its proliferation an urgent public health concern. The case underscores the critical importance of rapid diagnosis and aggressive intervention, as delays in treatment can render the infection universally fatal.
A Battle Against Time: The Man’s Ordeal
The unnamed patient’s ordeal began subtly, likely after exposure to brackish water, a common habitat for V. vulnificus. While the exact moment of infection remains unstated, these bacteria typically enter the body through open wounds or by consuming contaminated raw or undercooked seafood. Once the bacterium infiltrated his system, it unleashed a rapid and aggressive assault. V. vulnificus is notorious for its ability to cause necrotizing fasciitis, a severe infection that destroys tissue, fascia, and muscle. For this man, the progression was alarmingly swift, transforming an initial localized infection into a systemic crisis.
Upon arrival at the hospital, the severity of his condition was immediately apparent. His right leg was so extensively damaged by necrotic tissue—dead or dying cells and tissues—that it was beyond salvageable. The irreversible destruction necessitated an above-the-knee amputation, a drastic but life-saving measure. Simultaneously, his forearm, also ravaged by the infection, required extensive skin grafting, with healthy tissue harvested from other parts of his body to reconstruct the damaged areas. This aggressive surgical intervention, coupled with an intensive antibiotic regimen, proved to be his salvation. After six months of arduous healing and rehabilitation, doctors reported a remarkable recovery, a testament to the swift, decisive actions taken by the medical team, albeit at the cost of a limb. His survival stands in stark contrast to the grim statistics associated with delayed treatment for such severe V. vulnificus infections, where mortality rates can reach a staggering 100 percent.
The Molecular Arsenal of a Deadly Threat
Vibrio vulnificus is not merely a bacterium; it is a highly evolved pathogen armed with a sophisticated arsenal of molecular munitions. These include a variety of potent toxins and enzymes designed to overwhelm host defenses and exploit biological systems for its survival and proliferation. Once inside the body, these molecular weapons enable the bacteria to:
- Hijack Cells: They manipulate host cellular processes, turning them against the body.
- Siphon Nutrients: They efficiently extract essential nutrients from host tissues, depriving the body’s cells while fueling their own rapid growth.
- Degrade Structural Proteins: Enzymes break down vital proteins like collagen and elastin, which provide structural integrity to tissues and organs. This degradation contributes directly to the "flesh-eating" aspect of the infection, leading to rapid tissue destruction.
- Break Down Tissue Linings: They compromise the integrity of protective tissue barriers, allowing the infection to spread rapidly and deeply.
- Make Blood Vessels Leaky: Toxins can damage the endothelial cells lining blood vessels, causing them to become permeable. This leads to fluid leakage into surrounding tissues, resulting in swelling, reduced blood volume, and potentially hypovolemic shock, a life-threatening condition where the body cannot pump enough blood to meet its needs.
- Fuel Destructive Inflammation: While inflammation is a natural immune response, V. vulnificus can trigger an overzealous and dysregulated inflammatory cascade that, rather than clearing the infection, causes collateral damage to healthy tissues.
- Suppress Immune Defenses: Some bacterial factors actively interfere with the host’s immune cells, weakening the body’s ability to fight off the infection, thereby allowing the bacteria to multiply unchecked.
- General Tissue Destruction: The cumulative effect of these mechanisms is widespread tissue necrosis, leading to organ failure and, if untreated, death.
This multi-pronged attack explains the rapid onset and severe pathology of V. vulnificus infections, often manifesting as necrotizing fasciitis, severe sepsis, or primary septicemia following the consumption of contaminated seafood.
A High Price: Mortality Rates and Risk Factors
The overall mortality rate for V. vulnificus infections is approximately 35 percent, a figure that already places it among the deadliest bacterial infections. However, this mortality rate escalates dramatically for individuals with specific underlying health conditions. For anyone infected who also has an immunocompromising condition—such as HIV/AIDS, cancer, organ transplant recipients on immunosuppressants, or individuals with autoimmune diseases—or a pre-existing liver condition like cirrhosis, hepatitis, or hemochromatosis, the mortality rate can soar to 50–60 percent. The reason for this heightened vulnerability lies in compromised immune systems, which are less able to mount an effective defense against the aggressive pathogen. Additionally, V. vulnificus thrives in iron-rich environments, and individuals with liver conditions often have elevated iron levels, creating an ideal breeding ground for the bacteria.
Likewise, for those who develop sepsis—a life-threatening reaction to an infection characterized by a widespread inflammatory response that can lead to organ damage and shock—mortality is also about 50 percent. Sepsis is a medical emergency that requires immediate intervention, as its progression can be rapid and irreversible. For patients like the man in this case, where the infection progresses to severe tissue necrosis, if antibiotics or surgical removal of the necrotic tissue is delayed, the mortality rate tragically jumps to 100 percent. This grim statistic underscores the absolute necessity of prompt medical attention and aggressive treatment strategies.
According to the Centers for Disease Control and Prevention (CDC), Vibrio infections, collectively, cause an estimated 80,000 illnesses and 100 deaths in the United States each year. While Vibrio vulnificus accounts for a smaller number of these cases, it is responsible for the vast majority of Vibrio-related deaths, solidifying its reputation as the most lethal species within the genus.
Climate Change: Fueling the Spread of a Deadly Pathogen
The case of the man’s infection is not an isolated incident but rather a potent illustration of a growing public health crisis exacerbated by global climate change. Medical experts and environmental scientists are increasingly recognizing the direct link between a warming planet and the proliferation and geographic expansion of V. vulnificus.
-
Rising Water Temperatures: V. vulnificus thrives in warmer waters, with optimal growth temperatures typically ranging from 20°C (68°F) to 40°C (104°F). As global ocean temperatures continue to rise, coastal waters, estuaries, and brackish environments become increasingly hospitable to these bacteria for longer periods throughout the year. This extended period of favorable conditions allows bacterial populations to flourish, increasing the likelihood of human exposure. Data from the National Oceanic and Atmospheric Administration (NOAA) indicates a consistent upward trend in sea surface temperatures across the globe, directly correlating with the observed increase in Vibrio prevalence.
-
Geographic Spread: The warming of coastal waters has enabled V. vulnificus to expand its geographic range into regions where it was previously considered rare or nonexistent. Historically, the bacterium was predominantly found in warmer waters of the Gulf Coast and the southeastern United States. However, between 1998 and 2018, US cases of V. vulnificus increased eightfold, notably expanding into northern latitudes. This expansion includes states like Massachusetts, New Hampshire, and Maine, areas that traditionally experienced cooler waters. This shift suggests a northward migration of the bacterium’s habitat, making infections a potential risk for populations unaccustomed to such threats. A study published in Scientific Reports in 2023 projected a significant increase in Vibrio infections along the U.S. East Coast, with the pathogen potentially reaching as far north as New York within the next decade under current climate warming trajectories.
-
Storm Surges and Extreme Weather Events: Climate change is also leading to an increase in the frequency and intensity of extreme weather events, including hurricanes and storm surges. These events can dramatically alter coastal environments, leading to greater mixing of fresh and saltwater, increased runoff of pollutants, and the displacement of Vibrio populations into areas of human activity. The disruption of infrastructure and sanitation systems post-storm can also increase exposure risks.
-
Salinity Changes: V. vulnificus prefers brackish water, a mix of fresh and salt water commonly found in estuaries and coastal lagoons. Changes in salinity, whether due to increased freshwater runoff from heavy rainfall or sea-level rise altering coastal hydrology, can create more extensive and persistent brackish environments ideal for Vibrio growth. This dynamic shifting of salinity gradients directly influences the pathogen’s habitat availability.
-
Algal Blooms: Warmer waters and increased nutrient runoff often contribute to the formation of harmful algal blooms (HABs). These blooms can create anoxic conditions and stress marine ecosystems, which in turn can favor the growth of certain bacterial species, including Vibrio. The decomposition of these blooms can also release nutrients that further support bacterial proliferation.
The doctors involved in the man’s case explicitly articulated this concern: "The abundance and geographic range of V. vulnificus is projected to increase owing to factors related to climate change, including rising water temperatures, storm surges, salinity changes, and algal blooms." This statement from medical professionals treating the direct consequences of the bacteria underscores the scientific consensus on the matter. Furthermore, the increasing threat of antibiotic resistance, a global health challenge, complicates the treatment of all bacterial infections, including those caused by V. vulnificus, potentially making future cases even more difficult to manage.
Public Health Response and Expert Warnings
In light of the escalating threat, public health agencies and medical communities are emphasizing the urgent need for increased awareness, enhanced surveillance, and proactive prevention strategies. The CDC and state health departments are actively monitoring the spread of Vibrio infections and issuing advisories. Infectious disease specialists and epidemiologists infer that a key aspect of the official response must involve educating both the public and healthcare providers about the changing epidemiology of V. vulnificus. For healthcare professionals, this means a heightened index of suspicion for Vibrio infections, particularly in patients presenting with severe skin and soft tissue infections or septicemia after exposure to coastal waters or raw seafood, even in regions where the bacteria were historically uncommon. Early diagnosis through specific laboratory tests and prompt initiation of appropriate antibiotics are crucial.
Prevention and Protection: Mitigating the Risk
The Centers for Disease Control and Prevention (CDC) offers clear and actionable advice to minimize the risk of Vibrio infections:
- Food Safety:
- Thoroughly Cook Seafood: Only consume seafood, particularly shellfish like oysters, that has been thoroughly cooked. Raw or undercooked seafood can harbor Vibrio bacteria, which filter feeders like oysters can concentrate in their tissues.
- Wash Hands: Always wash your hands thoroughly with soap and water after handling raw seafood to prevent cross-contamination.
- Wound Care and Water Exposure:
- Avoid Water with Open Wounds: If you have an open wound, cut, scrape, or recent surgical incision, avoid entering brackish water, estuaries, or coastal marine environments. This includes swimming, wading, or engaging in any water-related activities.
- Cover Wounds Tightly: If unavoidable, ensure any open wounds are completely and tightly covered with a waterproof bandage.
- Immediate Wound Washing: If you sustain a wound while in brackish water, or if an existing wound is exposed to such water, wash it immediately and thoroughly with soap and clean, running water.
- Additional Precautions:
- Wear Protective Gear: Individuals who handle raw seafood or work in marine environments, especially those with pre-existing health conditions, should consider wearing protective gloves and footwear.
- Seek Medical Attention Promptly: If you develop symptoms such as fever, chills, blistering skin lesions, or severe stomach pain after consuming raw seafood or after exposure of a wound to brackish water, seek immediate medical attention. Inform your healthcare provider about your recent exposures.
Looking Ahead: A Growing Public Health Challenge
The escalating threat of Vibrio vulnificus is a complex public health challenge intertwined with the broader crisis of climate change. The case of the man who survived amputation underscores the bacterium’s devastating power and the critical window for intervention. As global temperatures continue to rise, the geographic reach and seasonal activity of V. vulnificus are projected to expand, increasing the risk of infection for more populations. This necessitates a multi-faceted approach involving robust environmental surveillance, enhanced public health education campaigns, and continued medical research into effective treatments and prevention strategies. Proactive measures, from individual adherence to food safety and wound care guidelines to broader governmental initiatives addressing climate change, are essential to mitigate the growing danger posed by this formidable marine pathogen and protect public health in an era of unprecedented environmental shifts.








